What is hepatitis C?
Hepatitis C (hep C) is an infection of the liver, caused by the hepatitis C virus (HCV).
What are the symptoms of hep C?
- Loss of appetite
- Stomach pain
- Tiredness
- Nausea
- Vomiting
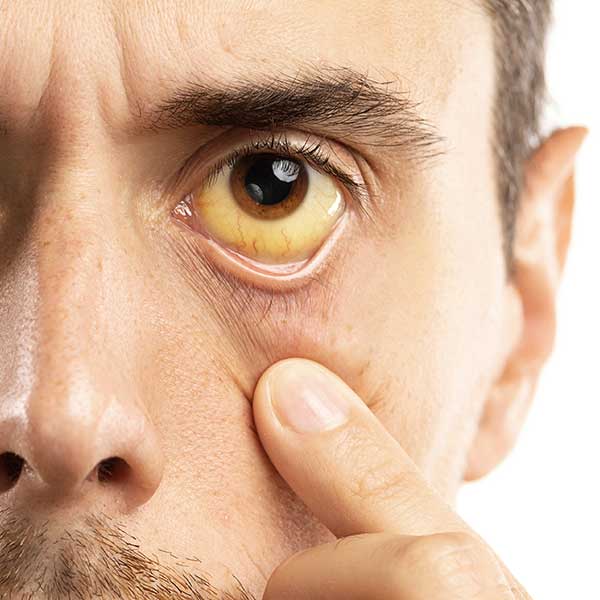
- Yellowing of the skin and whites of the eyes (jaundice)
Most people do not show any symptoms at all, but can still spread the germs to others without knowing it. Symptoms can take about 2 weeks to 6 months after the germs enter your body to show. By this time, the virus may have already caused damage to your liver. This is why it is important to take steps to prevent getting hepatitis C and get tested if you may have been exposed.
How does hep C spread?
Hep C spreads mostly through contact with the blood of someone with hep C infection. Common ways to spread the infection include:
- Sharing used needles or other drug equipment for injecting or inhaling drugs.
- Using contaminated medical, surgical, or dental equipment, such as insulin pens or tattoo needles.
- Being exposed by getting pricked by a contaminated needle or sharp at a workplace.
- Sharing personal items, such as toothbrushes, nail clippers, or razors.
It is also possible to spread hep C by having unprotected sex with an infected mother and from mother to baby during childbirth. The risk of getting hep C through blood and blood products is lower in Canada because donors are now screened for hep C infection. Hepatitis C is NOT spread by casual contact, such as hugging, kissing, shaking hands, or by being around someone who is sneezing or coughing. It does not spread by breastfeeding unless the nipples are cracked and bleeding.
Until your health care provider tells you that you have cleared the germs from your body, you can spread it to others. People living or travelling to countries where it is common are at a higher risk of getting hep C.
What are complications of hep C?
Some adults will recover within 6 months (known as acute hepatitis C infection). However, most will develop chronic infection, where the virus remains in their body for life. People who have chronic hep C can develop serious liver problems, such as liver scarring (cirrhosis) and cancer.

How do I get tested for hep C?
A simple blood test is collected by a health care provider to test for hep C. Some clinics may be able to do a point-of-care test, where they take a pinprick of blood. The results only takes 20 minutes to show. If the first test is positive, you will need additional blood tests to see if the virus is in your blood and see if you have recovered from the infection.
How is hep C treated?
- If you have these symptoms, see a health care provider as soon as possible. Tell your health care provider about any substance use and if you or your partners have been travelling.
- Tell your health care provider if you are pregnant or think you may be pregnant.
- In the first six months of getting hep C, some people will clear the germs without needing treatment. If the body cannot clear the germs on its own, a healthcare provider might order treatment.
- Hep C treatment can cure most people. Treatment includes a combination of antiviral pills (medications that fight against viruses). They are usually taken for 8 or 12 weeks. It is important to take the medication as prescribed by your health care provider. Many of the available medications are covered under the Ontario Health Insurance Plan (OHIP).
- Blood tests may need to be done before, during, and after treatment to make sure the medication is working.
- After recovering from a hep C infection, you are not immune to hep C. This means you can get re-infected.
What do I do if I have hep C?
Encourage all those who may have been exposed to your blood (e.g., sexual partners, people you live with) to get a test for hepatitis. The Health Unit can help you notify your partners, while keeping your identity confidential.
If you have not recovered from hep C, make sure to:
- Not share drug equipment, such as needles and pipes, if you use drugs. Dispose of used needles properly. Visit a local needle syringe program to get new needles, syringes, and other equipment.
- Practice safer sex and use barrier protection, such as condoms.
- Inform your doctor, dentist and other health care providers, about the infection so that they can take precautions.
- Not share personal items that may contain blood, such as toothbrushes, razors, or nail clippers.
- Not donate blood, semen, or tissues.
- Cover all cuts and sores.
- Clean up blood spills with diluted household bleach (9 parts water to 1 part bleach). Leave the bleach solution on the surface for 10 minutes before wiping it away. If others are cleaning up blood spills, make sure they wear protective gloves and wash their hands well after removing the gloves.
- Get tested for other sexually transmitted and bloodborne infections (STBBIs), such as HIV. Your health care provider may advise you to get the hepatitis A and B vaccines.
- Take care of yourself by eating a balanced diet, getting enough rest and exercise, and following up with your health care provider as needed. Avoid drinking alcohol to protect your liver.
How do I prevent hep C?
There is currently no vaccine to protect against hep C. Ways to prevent infection include:
- Not sharing personal items or drug equipment.
- Avoid dental, medical or cosmetic procedures that penetrate the skin (e.g., acupuncture, tattooing) unless you are certain that the needles, materials, and equipment are sterile.
- Practicing safer sex, such as:
- Abstinence (not taking part in any types of sex),
- Mutual monogamy (both partners only have sex with each other and have been tested for STBBIs, and
- Using latex and polyurethane male and female condoms and dental dams. Condoms are available for free at the Health Unit.
- Not sharing sex toys or thoroughly washing them with disinfectants between use
- Getting tested for STBBIs, if you had unprotected sex and/or are not sure if you or your partners have a STBBI.
For more information contact the Health Unit or speak to your health care provider.
- CATIE – Hepatitis C
- Government of Canada - Hepatitis C
- SexualHealthOntario (also has live online chat and Sexual Health Infoline): 1-800-668-2437
- Core Medical Centre Urgent Care Clinic
References:
CATIE. (2019). Hepatitis C: An in-depth guide. Retrieved from https://www.catie.ca/hepatitis-c-an-in-depth-guide.
Government of Canada. (2019). Hepatitis C. Retrieved from https://www.canada.ca/en/public-health/services/diseases/hepatitis-c.html.
Heymann, D.L. (Ed.). (2015). Control of communicable diseases manual (20th ed.). Washington, DC: American Public Health Association.
Ontario. Ministry of Health and Long-Term Care. (2019). Infectious diseases protocol, Appendix A: Disease-specific chapters, Chapter: Hepatitis C. Toronto, ON: Queen’s Printer for Ontario.

