Latest Updates
View Supervised Injection Services Community Consultations Report
FAQs:
SIS are provided at legally operated indoor facilities where people can come to inject their own drugs under safer conditions and supervised by trained workers. SIS are a harm reduction strategy, aimed at keeping people alive, safe, and healthy, even if they continue to use drugs. It gives them an opportunity to get treatment when they are ready. Some examples of harm reduction strategies are using a nicotine patch instead of smoking, needle syringe programs, or giving out naloxone kits to prevent overdoses.
Benefits of SIS include1,2,3:
- Less injecting in public spaces;
- Less tossing of used needles in public spaces;
- Greater access to withdrawal management and treatment and other health and social services;
- Less transmission of blood-borne infections, such as hepatitis C, through less needle sharing; and
- Reduced health care costs.



Locally in Windsor and Essex County (WEC), we are facing increased illnesses and deaths related to the use of opioids and other drugs:
- About 1 in 100 people reported that they have injected illicit drugs in their lifetime.4
- Opioids and methamphetamines are the second and third most common substances identified at emergency department visits in 2017.5
- There were 382 opioid-related emergency department (ED) visits in WEC in 2015, which is 3.6 times greater than in 2003. The rate in Windsor was 2.8-times greater than Essex County.6
- Emergency department visits related to methamphetamines has dramatically increased since 2013.5
- Number of drug-related overdoses in WEC increased from 505 in 2016 to 783 in 2017.7
- There were 37 opioid-related deaths in WEC in 2016; up from 24 deaths in 2015, 19 of which were in the City of Windsor.6
- The number of hepatitis C cases, a blood-borne infection, increased from 143 reported cases in 2016 to 181 reported cases in 2017.8
- In 2017, out of the 164 confirmed hepatitis C cases that reported at least one risk factor other than unknown, injection drug use was reported by 62% of cases (101 cases).9
- There have been 167 documented needle-related calls from January 1, 2014 to February 5, 2018 to local municipal services (3-1-1), predominantly in downtown Windsor.10
- Number of needle-related calls have significantly increased, from 43 in 2016 to 121 in 2017.10
- 3270 naloxone kits (a medication that reverses opioid-related overdoses) were given out between January 2017 to March 2018.11,12
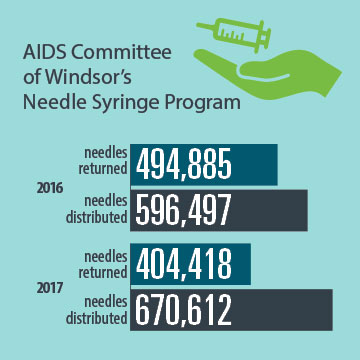
- The AIDS Committee of Windsor’s Needle Syringe Program reported 596,497 needles distributed and 494,885 needles returned in 2016. In 2017, the program distributed 670,612 needles, with 404,418 needles returned.13
SIS have been shown to address these public health issues and promote public safety. An exemption for medical purposes under the Controlled Drugs and Substances Act for activities at a supervised consumption site can be made by Health Canada, if there is a demonstrated need.
As part of the greater Windsor-Essex Community Opioid & Substance Strategy, community organizations are having conversations about SIS. No decisions have been made about providing SIS in Windsor.
Overdose prevention sites (OPS) are temporary sites that can operate for 3 – 6 months. These sites provide supervised injection, harm reduction supplies, and naloxone. They were developed in response to the opioid crisis because of the immediate need for health services to prevent illnesses and deaths related to drug use. OPS give communities time to plan and consult about more long-term solutions to addressing the needs of people who use drugs.
Supervised consumption services (SCS) are part of a long-term harm reduction approach. They are provided at legally sanctioned sites that can operate for longer, and offer more comprehensive services and education for people who use drugs than an OPS does. These include basic health services, testing for infectious diseases, and referrals to health and social services, such as treatment, rehabilitation and housing services. People who are ready to stop or want to reduce their drug use can also come and get support at these sites.
Supervised injection services (SIS) refer specifically to injectable drugs and are services provided at SCS. SCS includes all methods of consumption, including by injection, through the nose, and by mouth.
In fall of 2018, after a review of SCS and OPS, the Ontario Ministry of Health and Long-Term Care announced a new model, Consumption and Treatment Services (CTS), to replace SCS and OPS models. This model offered the same services, but emphasized the need for community consultation, availability of health and social services, and ongoing monitoring and reporting.
More information here regarding SCS, SIS, and OPS and here regarding CTS
No, there has not been a decision to offer SIS. There has been conversation among community partners about SIS. Before an exemption can be applied for, extensive assessment and planning is required. The purpose of this community consultation is to get feedback from the community to see if there is a need, what these services should look like, if potential clients would use such services, and if there are any concerns about SISs and how to address them. Tell us what you think by participating!
This is a common concern, and, as such, a lot of research was done on this from SIS operating in Canada, Europe, and Australia. There is currently no evidence of increased drug-related crime related to the operation of SIS in Europe and Canada. It is an important consideration when discussing SIS.
Yes, there are. Substance use is complex, and, as such, requires more than one approach. Looking at SIS as an option is only one part of a larger and comprehensive approach to substance use in Windsor. Community partners are working together to address prevention and education, other harm reduction strategies, treatment and recovery, and enforcement and justice related to opioid use. Some of these strategies include:
- Increasing provider and patient education on opioid use and pain management;
- Increasing access to naloxone kits to prevent overdose-related deaths;
- Advocating for increased funding to expand treatment services, while improving referral processes for people looking to access substance use services; and
- Developing community safety plans to protect those that are not using drugs, but are still directly impacted.
References:
- Kennedy, M.C., Karamouzian, M., & Kerr, T. (2017). Public health and public order outcomes associated with supervised drug consumption facilities: A systematic review. Current HIV/AIDS Reports, 14(5), 161-183. https://doi.org/10.1007/s11904-017-0363-y
- Ng, J., Sutherland, C., & Kolber, M.R. (2017). Does evidence support supervised injection sites. Canadian Family Physician, 63(11), 866.
- Wood, E., Tyndall, M.W., Lai, C., Montaner, J.S.G., & Kerr, T. (2006). Impact of a medically supervised safer injecting facility on drug dealing and other drug-related crime. Substance Abuse Treatment, Prevention, and Policy, 1(13). doi:10.1186/1747-597X-1-13
- Canadian Community Health Survey (CCHS) 2015-2016
- Ambulatory Emergency External Cause [2000-2017], Ontario Ministry of Health and Long-Term Care, IntelliHEALTH ONTARIO, Date extracted: [August 16, 2018]
- Windsor-Essex County Health Unit. (2017, June). Opioid misuse in Windsor-Essex. Retrieved from https://www.wechu.org/about-us/reports-and-statistics/opioid-misuse-win….
- Essex-Windsor EMS, Date received: [June 8, 2018]
- Windsor-Essex County Health Unit. (2018). Monthly infectious disease report – February 2018. Windsor, ON: Windsor-Essex County Health Unit.
- Integrated Public Health Information System (iPHIS), Ministry of Health and Long-Term Care, Date extracted: [June 8, 2018]
- City of Windsor, 3-1-1 calls, Date received: February 5, 2018
- Ontario Public Drug Program: Naloxone distribution in hospitals [2017-2018], Ministry of Health and Long-Term Care, Date received: [October 9, 2017]
- AIDS Committee of Windsor (ACW), Windsor-Essex County Health Unit (WECHU) and Windsor Essex Community Health Centre (WECHC) [Q1-Q4 2017]
- AIDS Committee of Windsor (ACW), Date received: [September 19, 2018]


